Modern medieval treatments: SPINAL FUSIONS
Weekly Book Recommendation:
“The only definitive book authored by Wim Hof on his powerful method for realizing our physical and spiritual potential.”
Research Article of the Week:
“the drive toward food is not only regulated by physiological needs, but is motivated by the pleasure derived from ingestion of food, in particular palatable foods. Therefore, feeding is viewed as an adaptive motivated behavior that involves integrated communication between homeostatic feeding circuits and reward circuits”
High on food: the interaction between the neural circuits for feeding and for reward
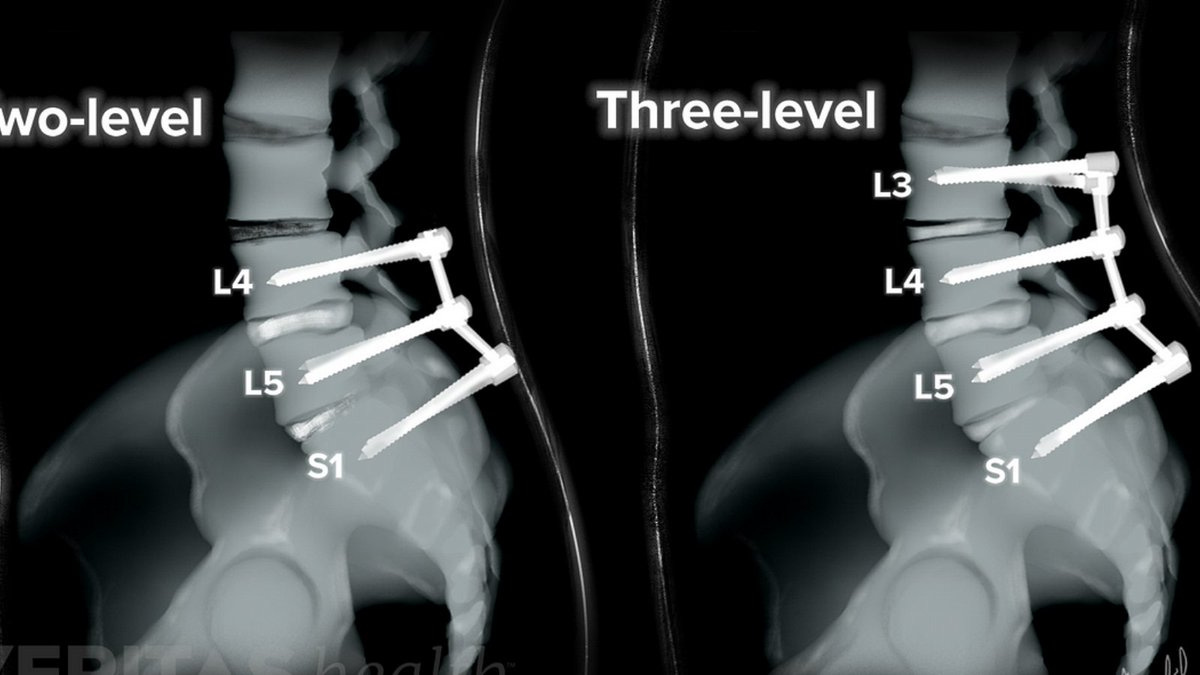
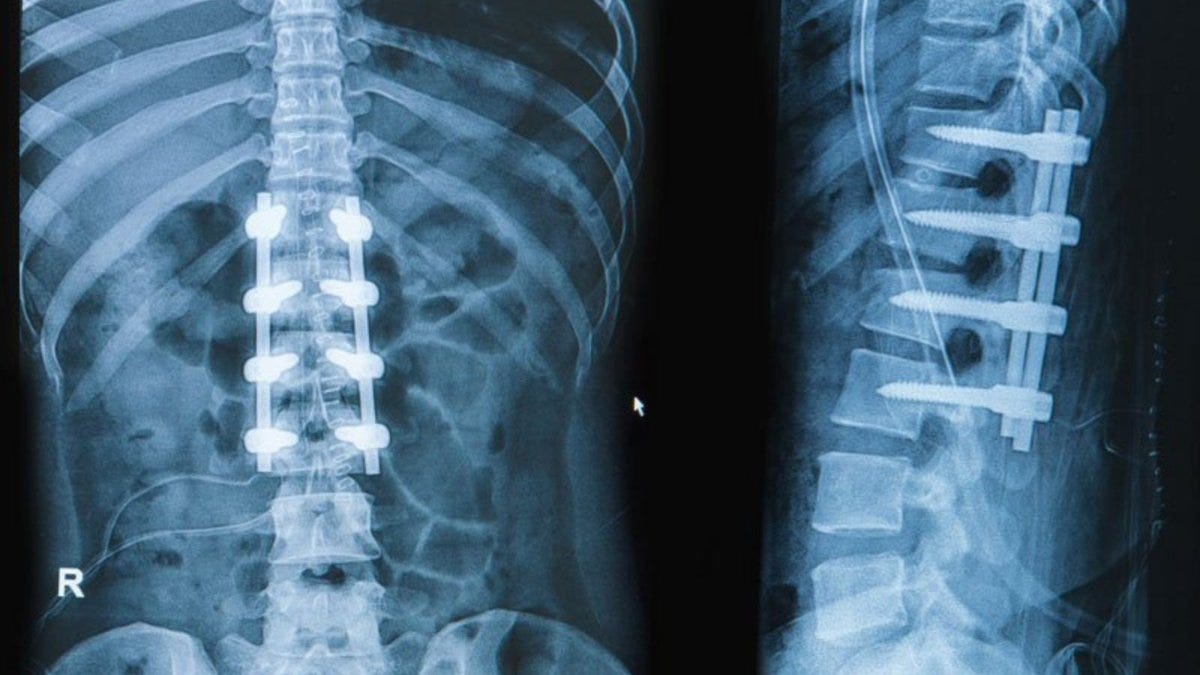
A spinal fusion is a surgery that uses hardware and screws to join two or more vertebrae, making a damaged section of the spine immovable. There are various types of spinal fusions with the goal of ultimately fusing together vertebrae in the spinal column.
Fusions are commonly performed when a patient has some type of degenerative disease, herniated discs, scoliosis, stenosis, or other injuries that cause pain or spinal instability. Over the past several decades, there has been an upward trend in the total number of spinal fusion procedures worldwide - associated with a high cost burden and risk of serious complications.
However, "science" does not always support the idea of fusions. Furthermore these surgeries have a massive effect o n the kinematics of the rest of the system.
“The present meta-analysis determined that fusion surgery was no better than nonoperative treatment in terms of the pain and disability outcomes at either short- or long-term follow-up.”
“Marked postoperative alterations were predicted in adjacent segment kinetics that depended on the preoperative L4–L5 disc condition, postoperative lumbopelvic kinematics and, to a lesser extent, the postoperative changes in the L4–L5 segmental lordosis and intraoperative muscle injuries. Moreover, upper (L3–L4) and lower (L5–S1) adjacent segment kinetics were affected post-fusion to different degrees.”1
Unfortunately, medicine often views the body in a reductionist manner, and gym training is often applied in a simplified way. For example, "fix the one disc in the low back, strengthen the core, or the biceps muscles". These are absolute biomechanical fallacies.
In reality, human movement is a complex orchestration of many different systems, all connected by fascia. See the substack below:
Anatomy views the spine as a series of blocks stacked on top of each other. These blocks are stacked with discs between each vertebra, "absorbing shock", and housing nerves and nerve roots. However this is only a good conceptual model, as the body is infinitely more complex.
Pain science also suggests the exact opposite of what is believed about fusions. For instance, often, there is no reliable correlation between physical abnormalities in the spine, such as slipped or herniated discs, and levels of physical pain. This has been proven repeatedly.
Most herniated discs de-herniate on their own over time, without medical intervention. Pain relief outcomes from interventions like back surgery are not significantly different from pain relief outcomes of more conservative approaches, even placebo. If you want to see more about placebo, nocebo, see below:
Our attitudes, feelings, and beliefs about back pain have a massive impact on the level of physical pain we feel. There are some broader topics about pain science that will certainly be covered in future newsletters.
There is very little high-level evidence that supports spinal fusions as truly effective. Although low-level studies have been published by spine surgeons/fusion-device manufacturers that seem to show that fusions may work, the caveat is, only for a short periods of time.
A team of physicians points out that "spinal fusion surgery efficacy for the most common indications, such as degenerative disk disease, remains unclear" at best.
Often patients elect for this procedure as a last resort because they are in severe pain or have been told their MRI "shows something". The truth is, the correlation between lumbar spine abnormalities found in MRIs and back pain is not that simple.
One study revealed that 32% of participants without lower back pain had 'abnormal' lumbar spines on their MRI scans, yet showed NO signs of pain. In contrast, 47% of participants with low back pain showed 'normal' lumbar spines, despite experiencing pain. What's even more compelling is that over the 12-month follow-up period, 13 subjects experienced low back pain for the first time, but showed NO change in their MRI results.
Based on these findings, the study concluded that "there was no clear relationship between the MRI appearance of the lumbar spine and [lower back pain]."
When we experience pain, we often want to find a simple answer or identify one specific thing causing it. For instance, it's easy to look at a herniated disc and immediately attribute it to the pain. Such thinking seems logical based on a causation understanding of pain.
However, as data suggests, these abnormalities are not always the direct cause of your pain.
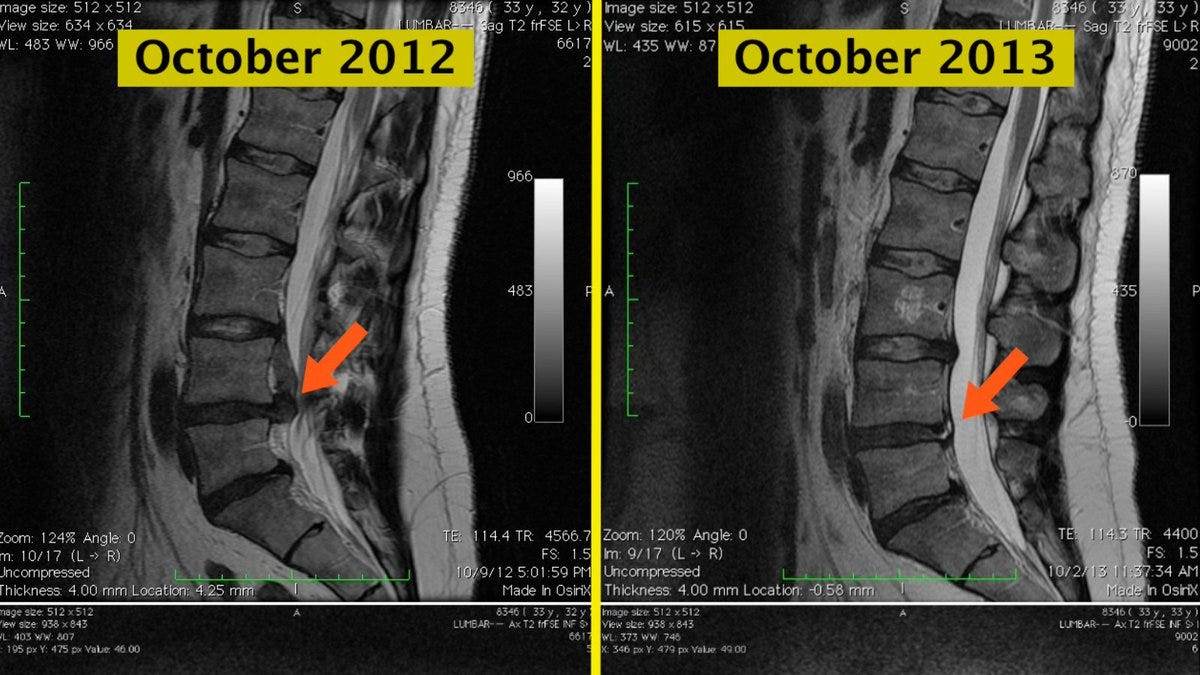
While MRIs can be powerful diagnostic tools, relying solely on them can be harmful to your pain perception. Many people ask whether a slipped disc can heal without surgery. The reality is that this occurs frequently, often without your knowledge. The medical community refers to this process as "Spontaneous Resorption," and it is the expected outcome for the majority of herniated discs.
Consequently, most physicians recommend a conservative "wait and watch" approach, rather than physical interventions. Research shows that "Spontaneous Resorption" applies to roughly two-thirds of all cases of herniated discs.2
However, some physicians prescribe physical therapy without taking into account the complexity of the body as a whole. Some physical therapists may just hyper-focus on the back or provide exercises that "strengthen the core". Others may even hand out pre-printed exercise sheets.
This approach overlooks the bigger picture and complexity of your body, and it's no wonder that cookie-cutter conservative treatments like this often fail. People may assume that their only option is an invasive, life-altering procedure.
That’s not to say that this procedure does not have a time and place - in a highly selective group of patients.3 However treatment indicates that surgical and postoperative rehabilitation interventions should focus on the preservation/restoration of patient’s normal segmental kinematics.
https://www.nature.com/articles/s41598-021-97288-2
https://pubmed.ncbi.nlm.nih.gov/33253955/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9609527/